Senior Drug Addiction, a Sensitive Issue
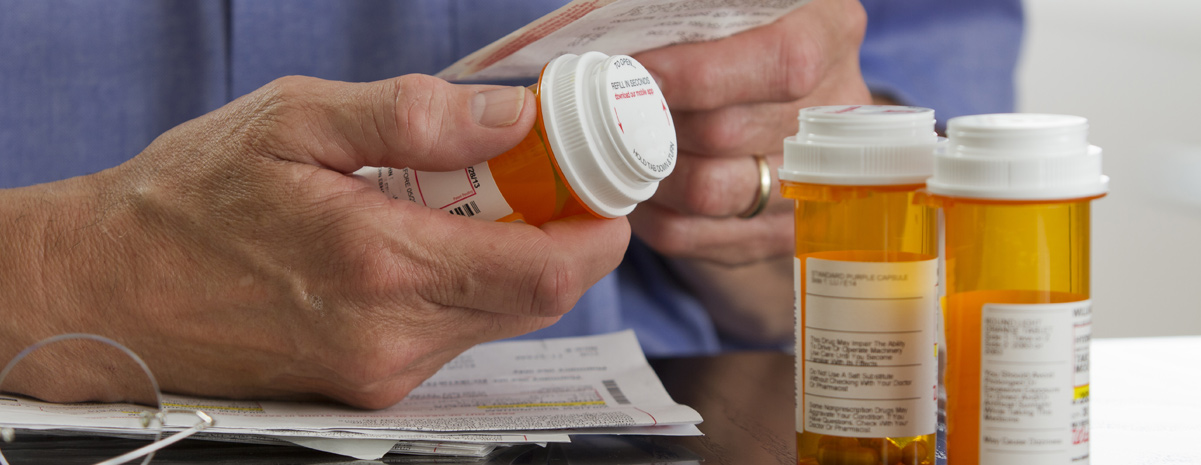
The Elderly and Substance Abuse
As a culture, we often underestimate both the extent and effect of addiction on our senior population. Though great headway has been made on educating the public that addiction is a disease, there is often an underlying assumption – or perception – of addiction as a problem afflicting only the young.
Certainly, you can imagine the likely affront if a senior citizen were asked to take a drug test on a routine visit to their physician. There is an undeniable sense that drug screening is used to rule out undesirable individuals from certain employment or to monitor felons on probation. It can seem undignified and even offense to drug test someone’s great grandmother.
No one wants to feel that a medical test is being undertaken because they are not trusted or are no longer competent to handle their own medication schedule.
Regardless of those facts, the elderly are at a real risk of harm from drug and alcohol misuse and abuse. Ultimately, ways must be found to normalize the expectation of drug testing, so that negative connotations are avoided and the true value of handing important knowledge to the physician is recognized.
Senior Exposure to Drugs and Alcohol
While teenagers often encounter drugs and alcohol as part of youthful rebellion and experimentation, at parties, or because of peer pressure, seniors come to addiction through different avenues. One thing both teens and seniors may have in common is attempting to self-medicate during stressful times or to overcome physical and psychological problems.
Both the young and old can identify with issues such as:
- The death of a friend, family member, or spouse.
- Loss of income and financial stresses.
- Family conflicts and trouble sleeping.
As we age, we not only find ourselves responding to these same stresses, but piling on a series of new ones as well:
- Retirement and loss of purpose.
- Relocation, perhaps to a nursing home.
- A decline in physical health, including major surgeries and diseases.
- A decline in metal health, including memory loss, depression, and dementia.
It’s easy to imagine a widow whose alcohol consumption increases during a period of grieving for a lost spouse, or a retiree whose sleep schedule becomes disrupted and tries to deal with it through prescription or over-the-counter sleeping medications, only to develop a dependency or exhibit dangerous sleep behaviors.
Today, one of the most commonly recognized senior addictions is related to the opioid crisis. For years, prescription opiates like Vicodin and Oxycontin were prescribed for pain in the elderly, often with the mistaken idea that they were not addictive drugs.
Now, imagine these same seniors seek medical attention for depression, weakness, short-term memory loss, or a variety of symptoms that may be related to aging, but which can also be caused substance misuse. Depending on other physical ailments, from back pain to diabetes, they end up visiting several doctors, all of whom may be ignorant of what the others are prescribing.
Even when seniors do report their medication schedules to each physician or medical practitioner in their lives, they should not be counted on to realize the consequences of forgetting, under reporting, or willfully concealing information.
According to the Office of Alcoholism and Substance Abuse Services, these scenarios would be classified as “late onset” drug abuse. Another group is the “hardy survivor,” a person who has been abusing drugs throughout their life and has simply aged into the senior population. In both cases, prescribing new treatments or drugs without an understanding of what substances the seniors are already dealing with presents a real danger to the health of the patient.
The Dangers of Undiagnosed Substance Abuse in Seniors
Aging presents many challenges, none of which are improved through the abuse of drugs or alcohol, whether or not that misuse is intentional. A clear example is any senior with mobility problems. Difficulty in walking or an unsteady gait already puts many at risk of falling. Introduce the effects of alcohol or pain medication and the risk of broken bones and hip fractures increases correspondingly.
According to a study by the Kaiser Permanente Center for Health Research, women aged 65 to 69 who break a hip are 5X more likely to die within a year than other women the same age. Each year over 300,000 older people are hospitalized for a hip fracture. Adding alcohol and drug addiction to the dangers of osteoporosis is neither a good recipe for prevention nor recovery from a fall.
Another danger is as simple as forgetfulness, a common complaint among older adults. Age related memory loss need not be a sign of dementia or Alzheimer’s disease, but it can be exacerbated by alcohol and drug use – which may then lead to not taking prescribed medications correctly.
A treating physician could be faced with a senior not taking needed medications properly or overdosing on the same prescriptions.
There are many possible scenarios where lack of awareness of an addictive behavior, or even the potential to cause addiction when one physician has prescribed sleeping pills, while another has prescribed pain medication, could result in a bad patient outcome.
The Value of Therapeutic Drug Monitoring
While it is natural to expect that grandmother may be taken aback, or your 80-year old uncle insulted, at the prospects of a drug screening, the value of placing accurate information in the hands of a physician can outweigh these concerns.
Ongoing testing during treatment can help provide an accurate picture of drug usage, which can be a life saver.
Therapeutic drug monitoring is an approach generally used in pain management scenarios. To be of use, therapeutic testing must go beyond screening for common drugs of abuse (DOA) and test at levels different than those typically used in drug screening scenarios.
Therapeutic testing must include drugs commonly prescribed for pain and sleep disorders, including opiates, methadone, benzodiazepines, and fentanyl. While urine testing is a fast and easy first step, blood testing is the best way of confirming a result and offering accurate quantization.
Armed with appropriate, quantitative information, physicians are better able to prescribe appropriately and address issues that may lead to or already have resulted in addiction among senior patients.
Extent of the Problem
Unfortunately, substance abuse among older adults is an invisible epidemic. According to a study by the National Center for Biotechnology Information (NCBI), abuse of alcohol and prescription drugs among adults 60 and over is one of the fastest growing health problems in the country.
The NCBI estimates drug abuse and misuse affects up to 17% of older adults. Today, that could represent an at risk senior population of over 8 million. And the problem will continue to grow. In 1990, only 13 percent of Americans were over 65. Estimates show that by 2030, older American will represent 21 percent of the population.
Senior health care systems and at-home services, already stressed by the continued growth of senior populations, can only be faced with greater challenges for each person who, instead of entering their golden years with a healthy head start, ends up battling addiction.
The Role of Ageism
We’ve already discussed the idea that seniors and their children or grandchildren may feel resentful or ashamed to even discuss the idea of addictive behavior. After all, isn’t drug abuse a failure of the young? Some elderly may have harbored judgmental feelings toward drug addiction all their lives, only to find themselves in a situation where denial is the obvious first choice.
Add to these problems the damage of ageism, where physicians and family may excuse behavior in older adults that would receive more attention in the young. This could be stated as the “how will grandma get through the day without her drink, or her pills,” phenomenon. “What does it matter, they won’t be here that much longer?” is another, more blatant way to see ageism in action.
Working to assure quality of life in older adults is about more than masking symptoms with pain pills or allowing older loved ones to slip into depression and alcohol.
Despite good intentions, ageism contributes to the fact that older patients are less likely to be diagnosed with substance abuse problems and less likely to receive treatment when diagnosed.
Addressing Pain in the Elderly
While over-prescription of opioids and the vast availability of alcohol play their roles, the one thing we should not lose sight of is that condemning the elderly to live in pain, either physical or psychological, is unacceptable.
Pain is not necessarily an inevitable result of growing old. It has both causes and consequences for daily living. It should also be recognized that many older people, rather than fake pain for attention and drugs, vastly under report pain. They may feel their pain is an inevitable part of aging, or they may believe reporting it will lead to an unwelcome diagnosis, such as cancer.
According to The Ochsner Journal, a multi-disciplinary approach to diagnosis and pain management is needed, because pain assessment in older adults can be complex.
A wide variety of options are available, depending on the diagnosis, from over-the-counter medications and topical analgesics to antidepressants and, yes, even opioids.
The goal, after all, is to improve quality of life for seniors and the elderly, and one way to do that is to find and ameliorate instances of drug and alcohol abuse and addiction.
To learn about Drug Testing Program Management (DTPM) and our turnkey services for laboratories in clinical, drug court, and physician’s office settings, call us today at 256-845-1261, or visit our Contact Us page today.







